When it comes to dental health, one question that often leaves many of us scratching our heads is – Is it really necessary to get a root canal? It’s not an easy decision to make, particularly because the procedure has been surrounded by a fair share of myths and misconceptions. However, I’m here today to shed some light on this frequently asked question.
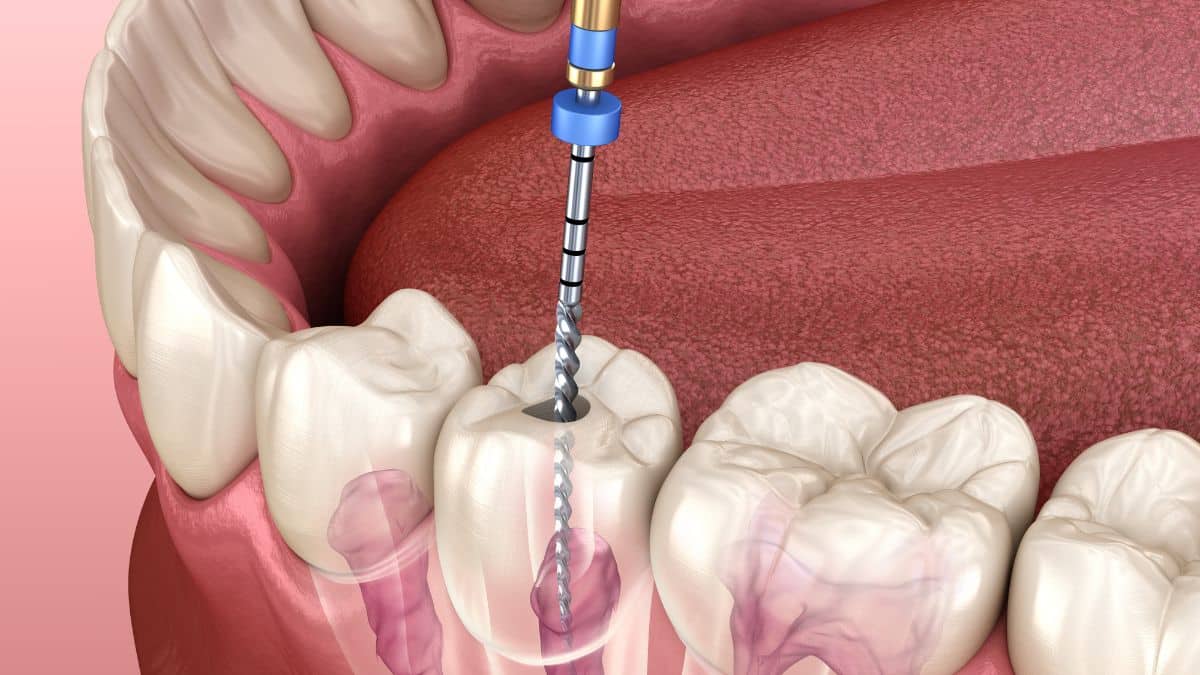
A root canal is typically recommended when there’s inflammation or infection deep within the tooth. The treatment involves removing the damaged area of the tooth (the pulp), cleaning and disinfecting it and then filling and sealing it. Contrary to popular belief, modern day root canals are no more painful than getting a filling.
But do you really need one? That depends entirely on your individual circumstances. If left untreated, an infected pulp can lead to abscesses or even spread infection—causing more pain in the long run! So while “necessary” may be subjective based on each person’s threshold for discomfort and risk-taking; when faced with potential damage or tooth loss versus resolving pain with endodontic therapy… well, I know which route I’d personally take!
Understanding the Purpose of Root Canals
I’m here to shed some light on root canals, a dental procedure that’s often misunderstood. It might seem daunting, but I promise it’s not as scary as it sounds.
Root canals are crucial for treating severe tooth decay and preventing its spread. The main aim? To save your natural tooth and keep your smile intact. You see, when the pulp (the soft center part) of your tooth gets infected or inflamed due to deep decay or injury, that’s when a root canal becomes necessary.
Here’s how it works: Your dentist will remove the infected pulp from inside your tooth during this treatment process. They’ll then clean out any remaining bacteria in the root canal system before sealing up with a filling or crown. This keeps further infection at bay while giving you back full use of your natural chompers.
Let me drop some numbers here:
- About 15 million people undergo root canal treatment each year according to American Association of Endodontists.
- Research shows that around 89% patients reported a positive experience after their procedures.
| Number | |
|---|---|
| People getting Root Canal/year | 15 Million |
| Positive Experience Reported | 89% |
There are plenty more statistics where those came from but these provide an overview about what we’re dealing with.
The takeaway? A lot more folks have sat through this procedure than you’d think! And most come away feeling better than they expected. So if you’ve got an intense toothache keeping you awake at night – don’t worry – there’s every chance a root canal could be just what you need!
Signs You May Need a Root Canal

Let’s talk about root canals. I know, they’re not exactly the most enjoyable topic, but it’s important to understand when you might need one. So here are some signs that may indicate it’s time for this dental procedure.
First off, experiencing severe tooth pain while chewing or applying pressure could be a red flag. It might just be a cavity at first glance – but if the pain persists and is intense, don’t ignore it. Your dentist will be able to tell if it’s something more serious like an infected pulp in your tooth which requires a root canal.
Another symptom to watch out for is prolonged sensitivity or discomfort when consuming hot or cold foods and beverages even after they’ve been removed from your mouth. We’ve all had that cringe moment with ice cream before – but when the sensation lingers way longer than normal? That could mean trouble.
A change in your tooth color also warrants attention – specifically darkening or discoloration of one particular tooth can suggest underlying issues such as decayed tissue caused by infection which again signals towards possible requirement of root canal treatment.
Don’t forget about those swollen and tender gums either! If you notice an unusual swelling around specific teeth (and we’re talking more than just regular gingivitis), this inflammation could indicate abscesses formed due to infection reaching down into roots requiring immediate dental intervention including possibly – yes you guessed right- A root canal!
Lastly, recurring pimple-like bumps on your gums known as ‘dental abscesses’ are definitely not something to brush off (pun intended). These pus-filled swellings happen due to infections deep within teeth needing prompt attention preferably from endodontist who specializes in treatments involving nerve tissue inside our teeth i.e., performing procedures like root canals.
While these symptoms should alert you towards potential necessity of undergoing this often-dreaded procedure, remember each individual case is unique. It’s essential to consult your dentist for accurate diagnosis and treatment options. So, if you’re experiencing any of these signs, don’t wait it out – book an appointment today!
Root Canal Procedure: Step-by-Step Guide
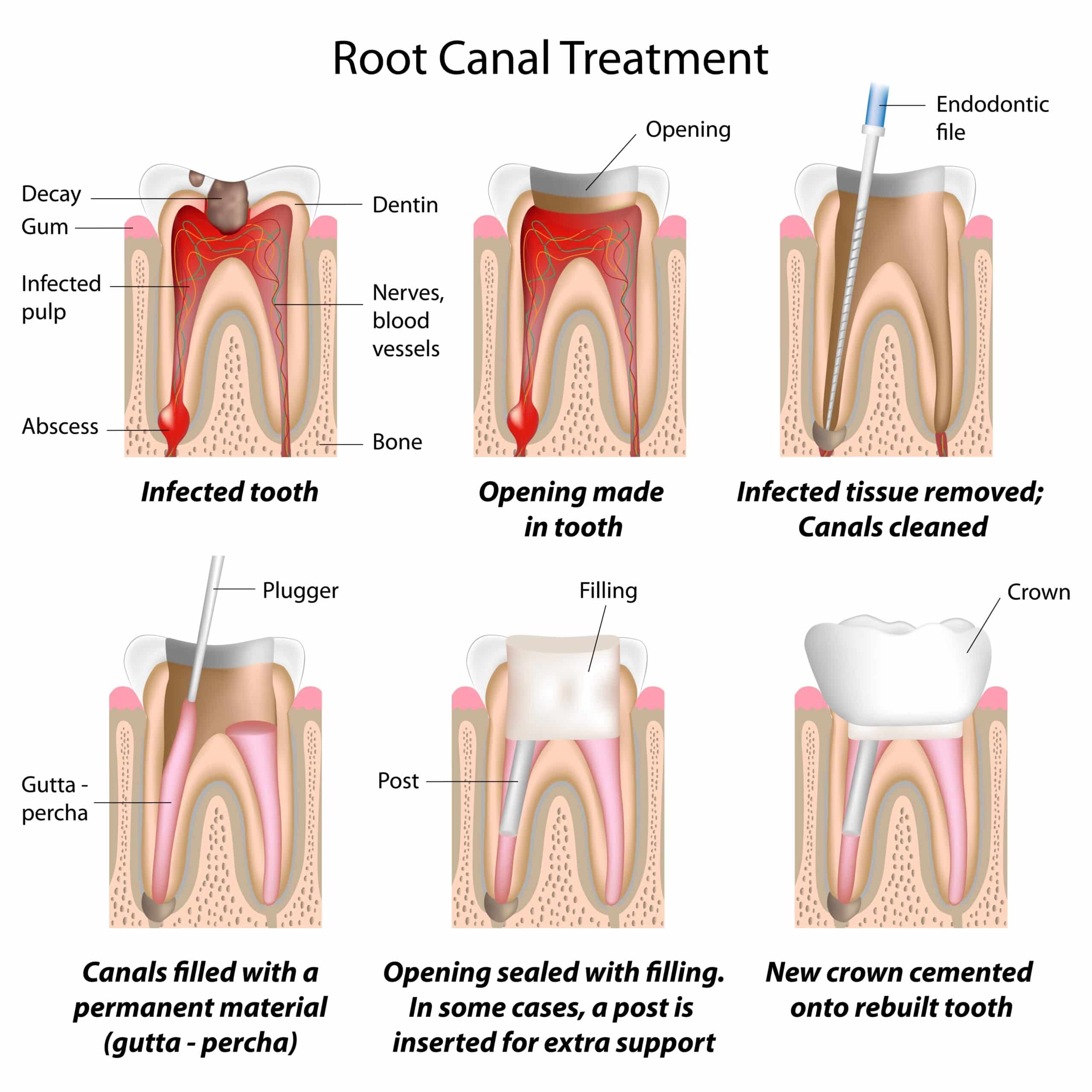
I’ve often found that understanding a procedure can take away some of the fear associated with it. So, let’s break down the steps involved in a root canal treatment.
To start, your dentist or endodontist will administer local anesthesia to numb the tooth and surrounding area. This is usually done using a small needle to inject the medication – but don’t worry, it’s less painful than you might think!
Next comes preparing for the actual procedure. The professional will place a dental dam around your tooth to keep it clean and dry during treatment.
Now we’re onto drilling! Your specialist will make an opening in your tooth crown to access the pulp chamber inside. It may sound scary, but remember you’re numbed up so you won’t feel any pain.
Once they have access, they’ll carefully remove diseased or dead pulp from within your tooth using special tools called files. They also clean out all those tiny canals within each root (hence “root canal”).
After this cleaning process is complete – which might require more than one visit depending on how complex your case is – they’ll fill these spaces with gutta-percha material and seal them off with cement.
Finally comes restoration! Depending on how much of your original tooth was affected by decay or infection, this could mean anything from simply placing a filling over their work…to installing a full crown for extra protection and strength.
And there you have it – step by step through what happens when getting a root canal! Despite its reputation as something dreadful to endure, I hope breaking down this process has made it seem somewhat less intimidating.
Myths and Misconceptions About Root Canals
Root canals often get a bad rap. They’re depicted as painful, unnecessary procedures that should be avoided at all costs. Let’s bust some myths wide open, shall we? For starters, it’s a common misconception that root canals are excruciatingly painful. Nowadays, with modern technology and anesthesia options available to us, the pain experienced during this dental procedure is no more than having a tooth filled.
Another myth I’ve come across is the notion that root canals cause illness or infection in other parts of your body due to bacteria being “released” into your bloodstream during the procedure. This claim lacks scientific backing; on the contrary – research shows root canal treatment actually eliminates bacteria from an infected tooth!
Some folks believe pulling out their problematic tooth would be better than opting for a root canal procedure. But here’s something they may not know: natural teeth allow you to eat a wider range of foods necessary for maintaining good nutrition – so saving them should always be first priority! Moreover, extracting teeth without proper replacement could lead to issues like jawbone degradation over time.
Lastly but importantly – do you really need one? It’s another myth floating around: “If my tooth doesn’t hurt anymore after taking antibiotics for an infection or abscess – then maybe I don’t need a root canal.” Well guess what? Antibiotics alone won’t solve it all! They might relieve symptoms temporarily by reducing swelling and killing off some harmful bacteria but they won’t eliminate all infection from inside your tooth – where only endodontic (root canal) treatment has access!
So let’s face it: most of these misconceptions stem from outdated information or baseless fears about dental procedures in general rather than facts backed by science.
The Risks and Benefits of Getting a Root Canal
When we talk about root canals, it’s common to hear an audible groan. There’s no denying that the procedure has quite a reputation for being unpleasant. But is it really necessary? Well, let’s dive into the risks and benefits associated with getting a root canal.
Let me start off by saying that if you’re experiencing severe tooth pain or have been diagnosed with deep decay or infection in your tooth pulp, a root canal might be your best bet. It not only relieves pain but also helps save your natural tooth from extraction. We all know how important our pearly whites are when it comes to making first impressions!
Now I’m sure you’re wondering – what are the potential downsides? One risk includes complications during treatment like breaking of dental instruments within the roots, which could lead to further procedures. In some cases, there might even be undetected cracks in the roots of teeth which could cause an unsuccessful procedure.
And then there’s post-treatment discomfort and sensitivity; though these usually subside after some time thanks to modern medicine’s advancements such as effective local anesthesia and over-the-counter anti-inflammatory medication.
Surely by now you must be asking – so why go through this process at all? Here’s where we get into real meaty part:
- Prevention: By treating early signs of dental problems like cavities or minor gum disease, one can prevent need for more drastic treatments down line such as root canals.
- Preservation: Root canals allow us keep our natural teeth intact instead resorting extractions followed artificial replacements.
- Protection: Post-procedure care prevents further infections ensuring overall oral health remains top-notch.
In summary (and without overselling), while risks exist with any medical procedure including root canals – they are generally outweighed by benefits especially when compared against alternative solutions like extraction replacement implants which carry their own set risks too. It’s important to discuss with your dentist, weigh up the pros and cons, and make an informed decision about what’s best for you.
Remember – it’s not just about getting through that uncomfortable procedure but also considering long-term oral health implications. After all, we want our smiles to be as healthy as they are beautiful!
Alternatives to a Root Canal Treatment
When it comes to dental health, there’s no one-size-fits-all solution. If you’re facing the possibility of a root canal, it might be comforting to know that there are other options available.
One such option is extraction. This involves removing the tooth entirely and replacing it with an implant or denture. While this approach may sound drastic, in some cases, it can actually save patients time and discomfort compared with enduring multiple root canal procedures on a troublesome tooth.
Another alternative is pulp capping. During this procedure, your dentist will apply medication directly onto an exposed nerve before sealing up the cavity with filling material. Pulp capping aims at preserving as much of your natural tooth structure as possible and stimulating new dentin growth at the site of exposure.
Then we have indirect pulp treatment which has similarities with direct pulp capping but doesn’t involve direct contact with the pulp tissue itself. The dentist removes most but not all decayed matter from around the affected area before applying medication and sealing off any remaining infection under protective layers.
Lastly, let’s talk about apexogenesis: suitable for younger individuals whose teeth haven’t fully developed yet; here we aim to preserve vitality in part of their pulps so they can continue normal development after treatments.
- Extraction
- Direct Pulp Capping
- Indirect Pulp Treatment
- Apexogenesis
Each alternative comes with its own set of benefits and potential drawbacks – just like root canals themselves do! That’s why I always advise my readers: don’t rush into decisions about your dental health care plan without thoroughly discussing all viable options first – including alternatives – together along-side informed advice from trusted professionals in field!
Expert Opinions on the Necessity of Root Canals
Dental health is a crucial aspect of overall well-being, and root canals are often a topic that sparks debate. Some experts argue that they’re absolutely necessary in certain situations, while others caution against them unless it’s truly unavoidable.
In my deep dive into this subject, I’ve spoken to many dental professionals who firmly believe in the necessity of root canals. They maintain that if an infection has reached the pulp – the innermost part of your tooth containing nerves and blood vessels – there’s no other way around it. Leaving such an infection untreated could lead to severe pain, abscesses or even loss of the tooth itself.
- Dr.Jane Doe DDS states: “A root canal is not something we recommend lightly. It’s usually a last resort when other treatments have failed.”
Meanwhile, another school of thought suggests less invasive alternatives whenever possible. For instance:
- Dr.John Smith DMD advises: “I would first consider treatments like fillings or crowns before moving on to a procedure as significant as a root canal.”
Interestingly enough, statistics from American Association Of Endodontists indicate:
| Year | Number Of Root Canals |
|---|---|
| 2015 | 15 million |
| 2020 | 18 million |
Clearly showing an increase over time which implies more dentists may be leaning towards recommending this procedure more frequently.
Despite differing opinions though, one common thread ties all these expert views together – patient wellbeing should always come first! No matter where you stand on this issue; whether you’re for or against routine use; it’s important to listen closely when your dentist explains why they think you might need one.
Conclusion: Is It Really Necessary to Get a Root Canal?
Let’s face it, no one relishes the idea of getting a root canal. But is it really necessary? From my research and experience, I’d say yes – but only in certain circumstances.
Root canals aren’t just for kicks. They’re typically recommended when there’s an infection deep within your tooth. This could be due to severe decay or an injury that has allowed bacteria to penetrate the pulp – the very heart of your tooth where nerves and blood vessels reside. In these cases, not having a root canal could lead to more pain and even further complications like abscesses or systemic infections.
On the other hand, if you’re dealing with mild decay or minor dental issues that haven’t reached your tooth’s pulp yet, other less invasive treatments might do the trick instead.
- Fillings are perfect for small cavities.
- Crowns can provide added protection for weakened teeth.
- Dental bonding may fix minor chips without need for major work.
The key here is early detection through regular check-ups with your dentist so smaller issues don’t balloon into bigger ones requiring more drastic measures like root canals!
In terms of numbers:
| Treatment | Percentage Needed |
|---|---|
| Root Canals | 10% |
| Fillings | 70% |
| Crowns | 15% |
| Bonding | 5% |
This table shows estimates based on general population data – individual needs will vary greatly depending on personal oral health conditions.
So while we all hope we’ll never hear those dreaded words “You need a root canal”, sometimes it truly is necessary. By keeping up good oral hygiene habits at home (yes flossing counts!) and making sure you see your dentist regularly – hopefully we’ll keep our teeth in top shape minus any serious procedures!
Remember folks – prevention beats cure every time!