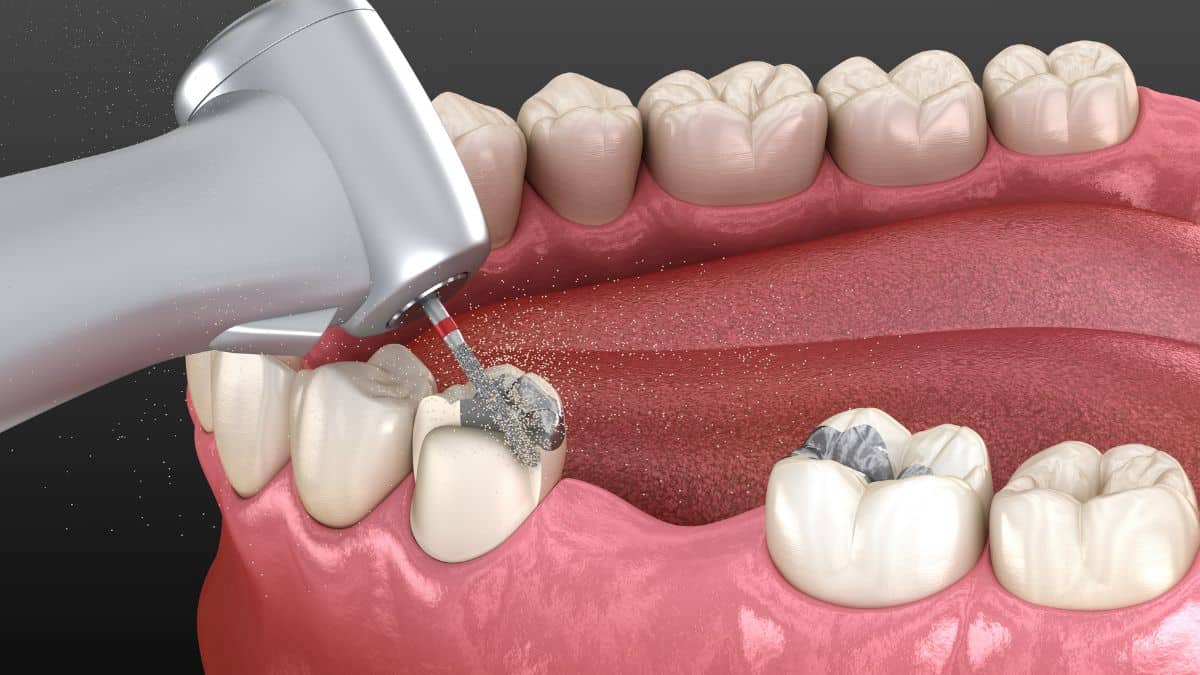
I’ve found that one of the most common questions people have when facing dental procedures is, “Will it hurt?” This concern is particularly relevant when we’re talking about getting a crown removed. It’s completely natural to feel apprehensive about any procedure that involves your teeth and gums.
Let me put your mind at ease: typically, having a dental crown removed isn’t painful. The process usually involves numbing the area around the tooth with local anesthesia so you won’t feel anything during the procedure. However, everyone’s pain tolerance varies and some might experience mild discomfort or sensitivity afterwards.
It’s important to remember this: dentists are professionals trained in managing pain and discomfort during dental procedures. They’ll do their best to make sure you’re as comfortable as possible throughout the entire process of removing your crown.
Understanding Dental Crowns: A Brief Overview
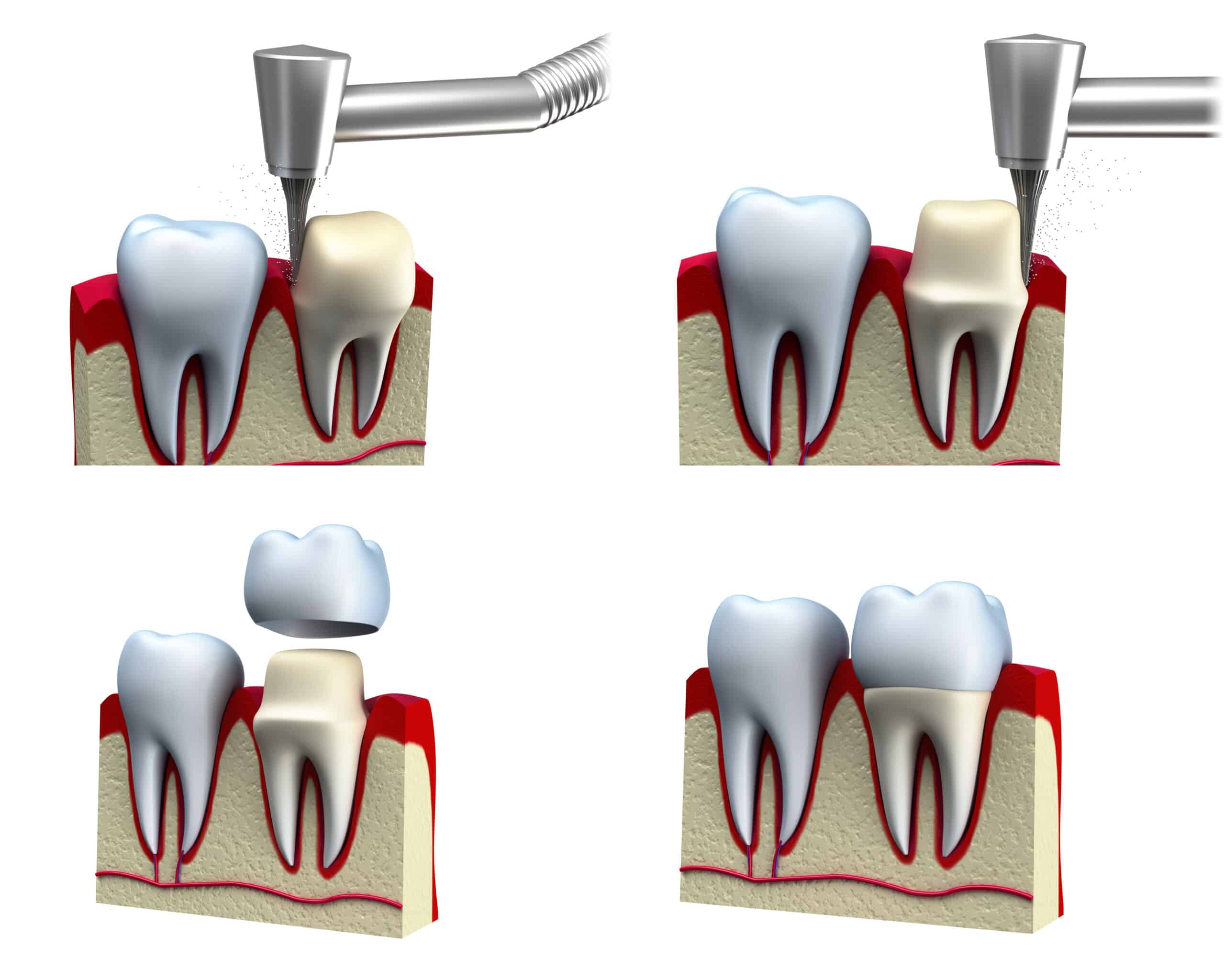
I’ll start by saying dental crowns are a common solution for various dental problems. They’re essentially caps that fit over a tooth, restoring its shape, size, strength and improving its appearance. You’ll typically find them in use when there’s a need to protect weak teeth from breaking or hold together parts of cracked teeth.
It’s essential to note that crowns can be made from several materials. These include stainless steel, metals like gold or other alloys (such as palladium), porcelain fused to metal, resin and ceramic. Each material has pros and cons depending on the patient’s needs.
For instance:
- Stainless Steel crowns are usually used temporarily while waiting for the permanent crown made from another material.
- Metal crowns withstand biting and chewing forces well lasting longer than other types.
- Porcelain-fused-to-metal gives color matching with your natural teeth but wear down over time.
- All-resin is less expensive but wears down faster
- And finally we have all-ceramic which provides better natural color match than any other crown type making it ideal choice for front teeth.
Dental crown procedure involves two visits at least to your dentist’s office: first one is preparation of tooth which might include X-ray examination followed by filing/shaping of tooth; second visit includes fitting permanent custom-made crown onto existing tooth after removing temporary one placed during initial visit.
Now you may wonder about lifespan of these restorations? Well I’m here to tell you that they generally last between 5 – 15 years based on material chosen along with oral hygiene practices & personal habits such as grinding/clenching etc.
So now you’ve got an idea about what dental crowns are all about! Keep reading though – we still need to talk about whether it hurts when they get removed…
The Procedure of Crown Removal: What to Expect
Before we delve into the specifics, let’s first understand what a dental crown is. A crown is essentially a cap that covers your tooth. Dentists typically use crowns when there’s significant decay or damage to restore function and aesthetics.
When it comes to removing a dental crown, the process isn’t as daunting as you might think. Your dentist will start by numbing the area around the tooth with local anesthesia. This ensures that you won’t feel any discomfort during the procedure.
Once your mouth is numb, they’ll use special tools to carefully loosen and remove the existing crown from your tooth. Depending on its condition – if it’s broken or severely damaged – this part can be somewhat tricky but rest assured that dentists are well trained for these situations.
Next up in line would be assessing and preparing your natural tooth underneath for a new crown fitting if required. This could involve cleaning out any decay present, reshaping through filing down or building up using filling material depending on what’s needed for optimal fit of new restoration.
Lastly, impressions of prepared teeth are taken which will serve as models for creating your new custom-made replacement crowns at lab.
Remember:
- You’re likely not going to experience severe pain during this procedure thanks largely due to local anesthesia.
- It may take several visits before everything gets completed i.e., removal of old one & placement of new.
- Following instructions given by dentist post-procedure can help ensure smooth recovery & longevity of newly placed restoration(s).
Factors That Can Influence Pain During Crown Removal

Let’s dive into the factors that can make crown removal a potentially uncomfortable experience. One primary factor is your personal pain threshold. It’s no secret that we all handle pain differently, and what might be a slight discomfort for one person could be more painful for another.
Another significant factor is the condition of your tooth under the crown. If there’s decay or infection present, it may cause increased sensitivity during the procedure. Additionally, if you’ve had root canal treatment on that tooth previously, it might affect how much discomfort you feel.
The dentist’s technique also plays an important role in this process. A skilled and experienced dentist knows how to minimize any potential discomfort during crown removal by using appropriate tools and techniques.
Consider these factors:
- Your individual tolerance to pain
- The state of your tooth underneath the crown
- The skill level of your dentist
It should also be noted that anxiety or fear about dental procedures can often amplify perceived pain levels. So staying relaxed during this procedure can go a long way towards minimizing any potential discomfort.
Lastly, it’s worth noting there are different types of crowns – metal crowns usually require less effort (and hence less potential for discomfort) to remove compared with porcelain or ceramic ones which are more firmly bonded onto teeth.
In essence:
- Anxiety levels
- Type of dental crown
Remember though: Regardless of these influencing factors, an experienced dentist will ensure they use local anesthesia as necessary making sure patients remain comfortable throughout their visit!
Managing Pain and Discomfort Post-Crown Removal
After having a dental crown removed, it’s natural to experience some discomfort. But don’t worry, I’ve got your back with tips and insights on how to manage any pain you might feel post-procedure.
Firstly, over-the-counter pain relievers are often sufficient for handling the mild discomfort that follows crown removal. Drugs such as ibuprofen or acetaminophen can be pretty effective in taming the pain. It’s important though to always follow dosage instructions listed on the package – too much of a good thing isn’t always beneficial!
For those who prefer a more natural approach, rinsing your mouth with warm salt water may help soothe irritated gums around the site where the crown was removed. This simple home remedy has been widely used for years because it works! The warmth of the water combined with salt’s healing properties can bring relief quite swiftly.
Remember also that cold compresses applied externally can help reduce swelling and numb any lingering pain in your jaw area after procedure. Just wrap an ice pack (or even frozen peas) in a thin cloth before applying it to avoid direct contact between ice and skin.
If these methods aren’t cutting it for you or if severe pain persists beyond few days post-removal – don’t hesitate reaching out to your dentist immediately! Prolonged intense discomfort could be sign of an infection or other complications which need professional attention ASAP!
All this being said: while there might be some level of unease following dental procedures like crown removals – know that there are numerous ways available for managing this temporary phase effectively until full recovery is achieved.
Preventing Potential Complications After a Crown Removal

After getting a crown removed, it’s not uncommon to experience some discomfort or sensitivity. However, there are several ways I can help you prevent potential complications and make your recovery as smooth as possible.
First off, it’s crucial to keep the area clean. This means brushing gently but thoroughly around the affected tooth and flossing daily. Remember that proper oral hygiene is your first line of defense against infection or other issues.
Pain relievers can also be handy during this time. Over-the-counter options like ibuprofen usually do the trick for mild discomfort post-procedure, but don’t hesitate to reach out if you’re in severe pain – that could be an indication of something more serious.
Another tip? Avoid hard foods until any sensitivity has subsided. Opt instead for soft foods that won’t put undue pressure on your tooth; think yogurt, soup, or scrambled eggs rather than crunchy veggies or tough meats.
Lastly – and perhaps most importantly – don’t skip follow-up appointments with me! These visits allow me to monitor healing progress closely and address any concerns before they become bigger problems down the road.
Here’s a quick rundown:
- Maintain good oral hygiene
- Use over-the-counter pain relievers if needed
- Stick with soft foods until sensitivity decreases
- Keep all follow-up appointments
With these measures in place after having a crown removed, you’ll be setting yourself up for success – minimizing risks while maximizing comfort during recovery!
When Should You Consider Getting Your Dental Crown Removed?
Deciding when to get your dental crown removed can be a tricky business. But, don’t fret! I’m here to guide you through this process. There are certain situations where it’s advisable or even necessary for the removal of a dental crown.
First off, if you’re experiencing consistent pain or discomfort around your crowned tooth, it might be time to talk with your dentist about removing the crown. Sometimes, a tooth under a crown can become decayed or infected and cause persistent discomfort.
Secondly, consider if there’s been damage to the dental crown itself. Has it chipped or cracked? If so, then its protective function is compromised and may warrant removal. Moreover, if you find that food keeps getting stuck around the area of your crowned tooth more often than not – this could indicate an issue with how well the crown fits onto your original tooth.
In some cases though – like visible wear on your crowns from years of use – replacement becomes inevitable rather than optional because worn-out crowns pose both aesthetic and functional problems in oral health care management.
Finally but importantly too: has there been any change in gum line exposing part of root surface? That’s another sign which indicates potential need for revisionary procedures including possibly having one’s current dental crowns taken off!
- Consistent Pain
- Damage (chips/cracks)
- Frequent Food Trapping
- Visible Wear
- Change in Gum Line
So remember folks: always pay attention to what’s happening inside mouth especially when already have something as significant as dental crowns installed; listen out for signs indicating trouble such as those listed above; consult regularly with trusted dentists about state-of-the-art methods available today ensuring optimal oral health maintenance!
Alternative Treatments to Dental Crown Replacement
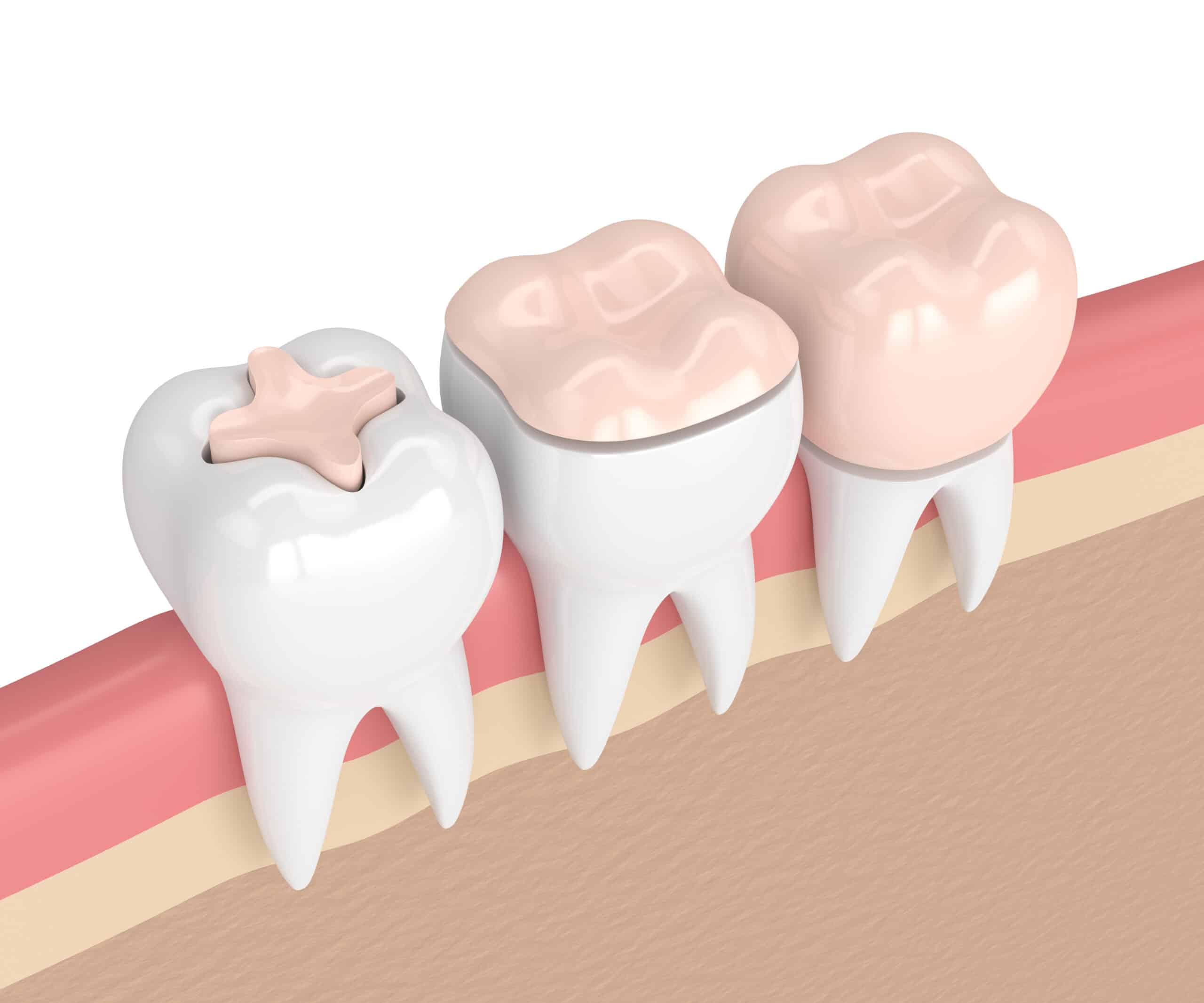
I’ll be honest, sometimes you’re not keen on the idea of having your dental crown removed and replaced. That’s alright; it’s completely normal to seek out alternatives that might cause less discomfort or suit your needs better. There are a few other options that you might want to consider if a crown replacement isn’t what you’re looking for.
One such alternative is inlays and onlays. These partial crowns can be a great choice when the tooth damage isn’t severe enough to require an entire crown but still needs some form of protection. Inlays fit within the tiny points, or cusps, of a tooth, while onlays cover one or more cusps.
Veneers also serve as another popular alternative treatment option. They’re thin shells made from porcelain or resin composite materials designed specifically for front teeth aesthetics improvement and minor shape corrections.
Dental bonding could be another viable option if there are small cosmetic issues with your teeth like chips, cracks, gaps between them or even discoloration. This involves applying a tooth-colored composite material directly onto the tooth which is then shaped and polished until it blends seamlessly with the surrounding natural teeth.
Lastly, let’s talk about dental implants – these are often considered when someone has lost their entire tooth due to injury or disease rather than just needing repair work done like in cases where crowns would typically be used.
Just remember: all these alternatives come with their own pros and cons too – they may not necessarily provide as much strength as traditional crowns do; some may take longer procedures while others could have higher costs involved depending upon various factors including complexity level required by each case.
Conclusion: Weighing the Pros and Cons of Removing a Dental Crown
Let’s face it, dental procedures aren’t exactly fun. They can be nerve-wracking, uncomfortable, and yes – sometimes painful. However, in some cases like removing a dental crown, it might be necessary for your oral health.
On one hand, you’ve got the pros of getting that troublesome crown removed. It eliminates any discomfort or pain caused by an ill-fitting or damaged crown. Not to mention how it can prevent further complications such as decay under the old crown.
On the flip side though are the cons that may come with removal:
- Potential pain during procedure
- The cost associated with replacement
- Time spent on multiple dentist visits
Here’s a quick look at these points:
| Pros | Cons |
|---|---|
| Eliminates discomfort | Potential procedural pain |
| Prevents further decay | Associated costs |
| Can improve oral hygiene | Time-consuming |
So what does this mean for you? Well ultimately, whether or not to remove your dental crown is something only you and your dentist should decide together. I recommend discussing all options thoroughly before making any decisions about your oral health care plan.
Remember to always keep communication open with your dentist about any concerns or questions regarding treatment options available to you.
In conclusion (and no pun intended), while removing a dental crown can indeed bring its share of challenges including potential pain during procedure; when weighed against benefits like improved comfort and prevention from further problems – it might just be worth considering after all!